|
According to Merriam-Webster, transfeminine people are whose gender identity is partially or fully feminine and differs from the sex the person had or was identified as having at birth; they are are people who were assigned male at birth (AMAB) but identify more with a feminine identity.
0 Comments
Our most recent MCI Youth Advisory Board member Meghana Reddy sat down with us to discuss her motivation in joining the board and her interest in male contraception. This blog post shares highlights from that conversation. In 2021, I decided that I wanted to start my own company focused on providing non-hormonal contraceptive options for women. Before starting my business, I created my own research protocol, and was able to interview over 50 individuals about the perspectives of contraception, sexually transmitted infections (STI)s, and the stigma surrounding sexual health. Because of the responses I received, I reached out to plenty of contraceptive pioneers, and was able to connect with Heather Vahdat, the Executive Director of Male Contraceptive Initiative (MCI). Through Heather, I was exposed to MCI's Youth Advisory Board (YAB), and decided it was the right fit for my interests and previous experiences. When I was conducting my personal research, I did not meet a lot of individuals that had an immense interest in contraception, until I met the individuals in the YAB. After joining the YAB in February 2021, I was able to learn more about new male birth control methods.
The critical work developing the next generation of non-hormonal, reversible male (or sperm-targeting) contraception is ongoing, and it is likely to be years before the first of these methods is available. Despite this, there are plenty of reasons to be excited about and optimistic for the future. These new methods will be transformational in ensuring reproductive autonomy for all, addressing significant challenges like unintended pregnancies, and helping meet the lofty sustainability goals necessary to improve the health of the planet and all its inhabitants.
There is no contraceptive “silver bullet” - no one method that everyone will see as the be-all-end-all of methods.
Imagine this - there’s an injectable contraceptive that lasts for a few months, but it requires seeing a provider, in their office, to administer the drug when it’s time. Or, alternatively, there’s a new daily pill, and it has almost no side effects, but it requires strict adherence to be efficacious, and missing a dose by even a few hours can be problematic. Or instead, imagine an option that works for years on end and is very effective, but requires a provider to make a small surgical incision in the scrotum during an administration procedure, and users would be sore for a few days afterwards. A persona is a fictional character created to represent a user type that might use a site, brand, or product in a similar way. They are incredibly useful tools in user-centered design, marketing, and other disciplines focusing on customers or “users”, and they are particularly useful during ideation activities for new products and services as they allow for the extrapolation of user preferences to inform attributes, thereby removing some of the ambiguity inherent in new product design.
Modern hormonal and prescription contraception is primarily focused on giving cisgender women, or people who identify as women who were also assigned female at birth, the means to protect themselves against an unintended pregnancy. While pills, patches, and IUDs are useful tools to help cis women control their fertility, they may fall short at protecting some cis men, trans, nonbinary, and intersex people. In recent years, there has been an increased awareness of sexual and reproductive health disparities adversely affecting LGBTQ populations.
Reproductive Autonomy For All
Male Contraceptive Initiative takes our mission seriously. We are constantly looking for ways to reach our goals and contribute to expansive contraception access. After an internal review of how we convey our values, MCI realized it was time to update. We have updated our vision to "Reproductive Autonomy for All." We believe that our work is more than just drug or product development. It's a mission to empower everyone with the freedom to choose how they manage their fertility, contraception, and family planning. With the global population continuing to grow and men’s options for contraception still limited to condoms and vasectomy, the time is ripe for another contraception revolution¹.
(Image courtesy of Pixabay) Each year, there are over 120 million unintended pregnancies experienced around the world, while the global population increases by over 80 million people. This constant human population growth has already translated to multiple significant challenges around the world, and will continue contributing to increased ecological degradation, conflict, climate change, natural disasters, global pandemics, and more. It is a reality that negatively impacts all of us. Consider this: unintended teen pregnancies in the United States are estimated to cost American taxpayers over $9 billion annually.
Our most recent intern from North Carolina Central University Edward Morris sat down with us to discuss his motivation in joining the team and his interest in male contraception. This blog post shares highlights from that conversation. Hello, my name is Edward Morris, I am a Public Health Education student at North Carolina Central University. I am a non-traditional student who had a prior career in the United States Army as a Bradley Commander and a Chemical Operations Specialist. I served 2 tours in Operation Iraqi Freedom. I wanted to continue to serve the American people and advocate for better health for underserved communities.
(Photo courtesy of Sansum Clinic) This blog post is written by Male Contraceptive Initiative's Youth Advisory Board Member Claudia Brewer When we hear “male birth control,” the vasectomy may be the first thing that springs to mind for many of us. Despite this, there’s a lot of confusion out there surrounding this procedure: Is it permanent, or reversible? Does it fulfill all of men’s contraceptive needs? To get to the bottom of these questions, I did some research and spoke with Dr. Alex Koper, a urologist at Sansum Clinic with 40 years of experience performing and counseling for vasectomies.
Male Contraceptive Initiative condemns in the strongest possible terms any and all acts of violence perpetrated against any group or individual. The most pressing reason for asserting this today is the unconscionable rise in attacks on people of Asian descent in America over the past year, with at least 3,700 individual acts of violence reportedly committed against this community since the start of the COVID-19 pandemic. We are saddened and distressed by this violence and the way it affects Asian American communities.
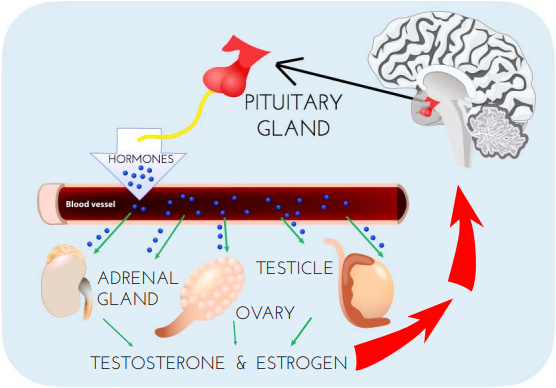
(Image credit: Dana Foundation - Illustration by Elizabeth A. Weaver II) Male Contraceptive Initiative provides funding and advocacy support for the development of non-hormonal, reversible forms of male contraception. But what does “non-hormonal” mean? How do these methods differ from “hormonal” contraceptives? In this post, we share a primer on the difference between hormonal and non-hormonal contraception.
A mandate for all physicians far and wide is “Do No Harm.” A mandate in which the health of the patient is prioritized above all else, and the health benefits of any treatment should outweigh the risks of that treatment. This creates a situation in which life-saving therapies with powerful and sometimes dangerous side effects are easily justified, because without treatment a very serious diagnosis could kill the patient entirely.
Our most recent MCI Youth Advisory Board member Claudia Brewer sat down with us to discuss her motivation in joining the board and her interest in male contraception. This blog post shares highlights from that conversation. What do you study/what's your academic background?I’m pursuing a B.S. in Molecular, Cell, and Developmental Biology with a Minor in Society and Genetics at UCLA. My goal in college is to gain a deep understanding of human health, from the complex molecular mechanisms underlying disease to the broader social and political implications of the latest bioengineering technologies. Most of my background is in biological research and healthcare. Most recently, I conducted research on a pathogenic protein associated with Alzheimer’s and other neurodegenerative diseases at the UCSB Neuroscience Research Institute. I currently serve as a scribe for a primary care physician at UCLA Health.
This blog post is written by Male Contraceptive Initiative's Executive Director Heather Vahdat, and is response to the article "The young women choosing to go without contraception" It’s Saturday and I’m supposed to be finishing a project that was meant to be a Christmas gift for my mother-in-law...last year. However, I allowed myself a quick look on the computer to find a sewing pattern I need and poof, here I am frustrated and writing a blog post. I can’t say I’m surprised that I find myself writing about contraception - it’s the classic “one quick peek at facebook/linkedin/wherever you saw the article couldn’t hurt”. But tell me, how can I not be distracted after seeing this article in my newsfeed?
Male Contraceptive Initiative’s mission is, “to empower men, and couples, to fully contribute to family planning goals by providing them the resources they need for reproductive autonomy.” It is how we articulate our most hopeful vision of the future: one where there is reproductive autonomy for all people. This vision and associated mission directs our daily activities, which encompass financial support to the male contraception research community and advocating for the development of additional male contraceptives.
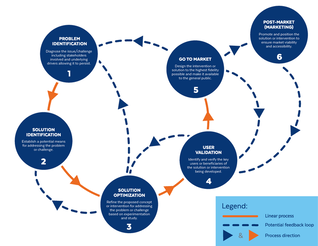
Introduction The drug development process is often presented as a linear process: you achieve one milestone before moving on to the next, with progress taking the developer ever forward. The Food and Drug Administration defines this process as such:
Based on the way that this information is conveyed, you might expect the process to visually represent something like this: This guest blog post comes is written exclusively for Male Contraceptive Initiative by freelance journalist Raizel Joleigh.
The topic of contraception can be contentious. Women have a host of options when it comes to birth control, and these come with their own dialogue that deserves an avenue of its own. For men, though, the only methods currently available on the market are condoms or vasectomies – unreliable and costly to reverse, respectively. This blog post is by Heather Vahdat, MCI Executive Director.
The National Center for Health Statistics at the Centers for Disease Control and Prevention (CDC) recently published a brief related to sexual activity and contraceptive use among young people between the ages of 15-19 in the United States. Given that young people are a key population for us at Male Contraceptive Initiative, I found the report to be interesting across the board; however, one key finding particularly caught my attention: “The condom remains the most commonly used contraceptive method among female teenagers”. In fact, 97% of female teenagers who have had sex reported ever having used a condom. We spend a lot of time at Male Contraceptive Initiative thinking about how best to accelerate the research and development of novel methods of non-hormonal, reversible male contraception. It is, unfortunately, a field that simply does not receive enough attention or funding, so it is up to us to ensure that our investments have the greatest impact possible, both in the short-term and the long-term.
Gathering and sharing the perspectives of those working in the male contraception field and general public is a communications and advocacy imperative at Male Contraceptive Initiative. It is critical to our mission that we seed and share conversations around the need and demand for novel methods of male contraception in order to ensure there is grassroots support while the work takes place to move these potential products from mere ideas to market realities.
The recent news coming out of India is cause for excitement amongst those interested in male contraception. Dr. Sujoy Guha and the rest of the RISUG team reported completing clinical trials in humans on the subcontinent, paving the way for access to the long-acting male contraceptive in India. News reports are saying that RISUG is now just waiting on final approvals from the Indian government, and that production could begin in as little as 6-7 months.
MCI Youth Advisory Board member Connie Dean sat down with her male partner, Riley, to talk though male contraception, unequal contraceptive burden, and what to do about it.
Whenever I first mention my work with MCI or even the notion of male contraception to my female friends, I am met time again with the same statement, “Oh men won’t take that, I don’t trust it.” I get it–we’re college students with our lives ahead of us, so this fear of pregnancy is self-preservation. Whether it’s individual experience or internalized social norms that conjure this fear and consequent knee-jerk rejection, the data shows that men would take contraception if it were available, and in fact they want it to be. Now, statistics are one thing, but in my quest to assuage the worries of my friends, I sought to humanize this side of the argument: I sat down with my (male) partner, Riley, to talk it through. The conversation around male contraception has been that it will be available “soon.” Multiple articles (such as this, this, and this) dating back to the early 2000s and further have claimed that a male pill is on the way. If the timeline that’s been promised is to be believed, we should all already be able to buy and use male contraceptives. Why can’t we?
|
Categories
All
Archives
April 2024
|
|
|
Donate to Male Contraceptive InitiativeYour generous donation makes a difference!
|
© Male Contraceptive Initiative. All rights reserved.






















 RSS Feed
RSS Feed
