|
Vaginal rings are a short-term, hormonal birth control method used by people with vaginas to prevent pregnancy. It is a flexible plastic placed within the vagina and releases hormones to disrupt ovulation.
0 Comments
This blog series highlights pertinent publications that were featured in MCI's monthly newsletter editions in the second quarter of 2023. The purpose of this blog is to report interesting or relevant work from MCI Fellows, Grantees, staff members, and other community authors in the field of male contraception.
It has been one year since The U.S. Supreme Court ruled to overturn Roe v. Wade, restricting Americans’ reproductive freedoms in a way that has not been seen for generations. Following the Dobbs decision that ushered in this curtailment of reproductive rights, there has been fear and speculation about what further steps might be taken to restrict individual reproductive autonomy.
Fertility is a way of preventing pregnancy through natural family planning. It is done by a woman monitoring and recording different fertility signs throughout her menstrual cycle to determine when she is most likely to get pregnant. She can prevent pregnancy by avoiding unprotected sex during her most fertile days through abstaining or implementing a barrier method.
A diaphragm is a barrier contraceptive device that covers the cervix to block sperm from entering. It is a cup made of soft latex, plastic, or silicone with a firm, flexible rim placed deep in the vagina before sex to prevent sperm from being able to reach an egg.
(Image courtesy of James Heilman, MD - Own work, CC BY-SA 3.0, https://commons.wikimedia.org/w/index.php?curid=22535295) The contraceptive patch is a small, flexible, adhesive patch worn on the body for 3 weeks, and is removed for the fourth week to allow for menstruation. The patch continually releases the hormones estrogen and progestin, which prevent ovulation and thicken the cervical mucus to prevent pregnancy.
The quest for effective and reliable male birth control methods has gained significant attention in recent years thanks to the efforts of organizations like MCI. While advancements in contraceptive options for women have also been substantial, the limited choices available to men underscore the need for innovative solutions in order to provide safe, effective contraception for all genders. Developing this next generation of birth control methods requires developing a deep understanding of people's needs and preferences, which is where market research plays a vital role: offering valuable insights that shape the design and development process. In this blog post, we will explore why understanding people's needs is crucial and make a compelling case for conducting market research in the realm of male contraception.
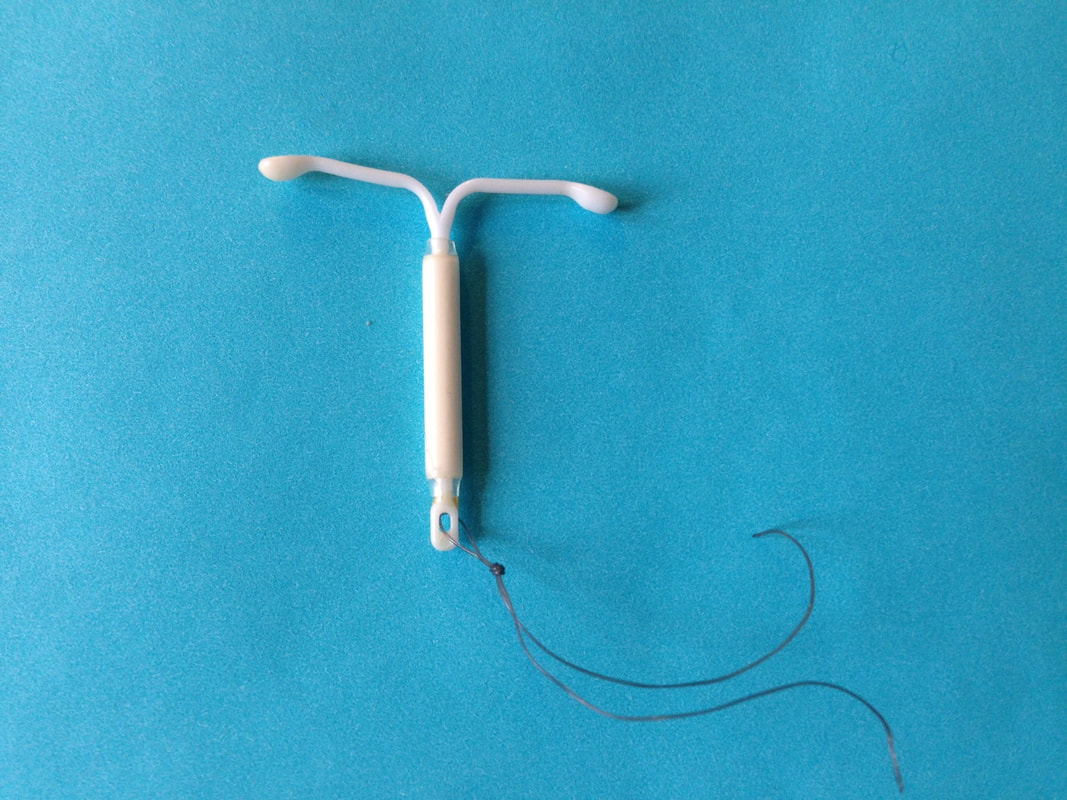
(Image courtesy of Sarahmirk, CC BY-SA 4.0 <https://creativecommons.org/licenses/by-sa/4.0>, via Wikimedia Commons) An Intrauterine Device, or IUD is a long-term contraceptive option placed within the uterus through the vagina by a healthcare provider to prevent pregnancy. It is a T-shaped, plastic device with one or two strings hanging from it that reach through the cervix into the vagina.
Reproductive autonomy is a fundamental human right that enables individuals to make informed decisions about their reproductive health and exercise control over their own bodies. Historically, the responsibility of contraception has been placed primarily on women, which limits their reproductive autonomy. However, male birth control has the potential to revolutionize reproductive health and empower all people to take control of their own reproductive choices.
This blog series highlights pertinent publications that were featured in MCI's monthly newsletter editions in the first quarter of 2023. The purpose of this blog is to report interesting or relevant work from MCI Fellows, Grantees, staff members, and other community authors in the field of male contraception.
With all the attention and excitement building about ChatGPT and the future of Artificial Intelligence-assisted, well, everything, we decided to put the platform to work and asked it to write a blog post for us about male birth control. Less than a minute after asking, here’s what it came up with:
(Image Source: Y. Rosen, MD) The production of sperm can be disrupted with a rise in temperature. Male thermal contraceptive methods (MTCs) involve heating the testicles inside the scrotum so that sperm production is slowed down. MTCs induce temporary infertility in men via a number of different methods, including applying hot water to the scrotum, generating heat on the testicles using ultrasound or heating pads, and creating artificial cryptorchidism (i.e., holding the testicles inside the abdomen) using specialized underwear.
This blog series highlights pertinent publications that were featured in MCI's monthly newsletter editions in the fourth quarter of 2022. The purpose of this blog is to report interesting or relevant work from MCI Fellows, Grantees, staff members, and other community authors in the field of male contraception.
The end of the year always invites the opportunity to look back and reflect upon all that transpired over the previous months that help define the year, whether good, bad, or otherwise. It is an opportunity to introspect and evaluate how yesterday’s actions led to today and help inform tomorrow.
A critical component of advancing the cause of “Reproductive Autonomy for All” is education. The shortcomings of sexual education are not limited, and are seemingly universally felt with disastrous results. As such, it is incumbent upon all of us to take the steps necessary to fully understand our reproductive biology in order to better inform our family planning objectives and to make the best decisions possible for our individual needs and desires.
Thankfully, there are a plethora of great resources available to help meet our educational interests and needs, including a whole host of books that both inform and inspire us here at MCI. In this post, we share a collection of our favorite books, but please also be sure to subscribe to our monthly newsletter as we highlight these and other titles periodically. GivingTuesday is a movement to create an international day of charitable giving at the beginning of each year’s holiday season. It’s a chance to both highlight and support nonprofits and charities dedicated to making the world a better place. We respectfully request that you consider supporting MCI on this holiday of giving by making a tax-free donation.
We believe that all people should have reproductive autonomy, and the access to contraception that works best for their bodies and their lifestyles. Unfortunately, not all people have this. We’re here to talk about a group of people who may not have access to contraceptive products that are safe and reliable in pregnancy prevention. Overweight and obese individuals that are sexually active deserve to have birth control that they can rely on and have access to.
Understanding people’s perspectives around male contraception helps guide our work at MCI. Sharing them is a privilege as well as a mandate: it’s of strategic importance to us to facilitate and broadcast the interest for male methods in an effort to present the undeniable market demand for them. Normally this is done through the lens of our grantees, fellows, research community, or even the general public. But lately, we’ve been endeavoring to share the views of MCI’s staff as well. In that spirit, this is a conversation with our Program & Communications Coordinator Sabey Boswell in which she shares her thoughts about male contraception as well as her interest in working with MCI.
This blog series highlights pertinent publications that were featured in MCI's monthly newsletter editions in the third quarter of 2022. The purpose of this blog is to report interesting or relevant work from MCI Fellows, Grantees, staff members, and other community authors in the field of male contraception.
September is Sexual Health Awareness Month. If your sexual health isn’t something you’ve thought about in a while, then now is a perfect time. We know that it can be hard to talk about these things, as there are a lot of stigmas surrounding sexuality. We’re here to shed some light on sexual health and encourage open conversation. If you want to have a healthier and more fulfilling sex life, this article is for you!
Vasectomy and condoms are the only current options for male contraception. The most popular form of long-acting male contraception is a vasectomy. Unfortunately, vasectomies are not considered truly reversible. Reversal of a vasectomy is often expensive, and requires a long surgery by a specialized provider.
MPTs or Multipurpose Prevention Technologies are products created to prevent unintended pregnancy and protect against HIV and other sexually transmitted infections. In order for a product to be labeled as an MPT, it must protect the user from at least two of the following reproductive health risks: HIV, STI transmission, and unintended pregnancy.
How does the law relate to reproductive health, especially male contraception? This is a question I found myself answering in many instances whenever I presented my topic to the lecturer for approval. For once, I thought this would be a unique experience; doing something that has been missing in my field of study and the feeling of being the first to explore the idea was overwhelming. Little did I know that I was getting myself into something that would shape my general perception and career projection.
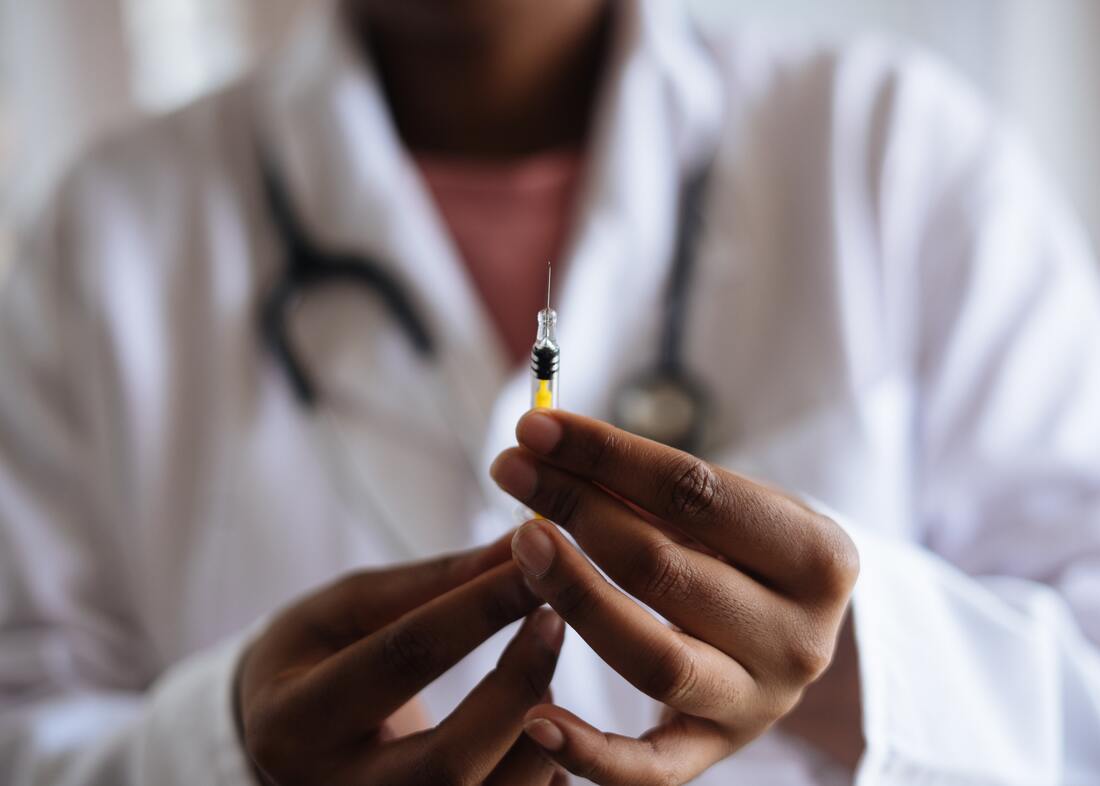
A contraceptive injection is a long-acting hormonal method that prevents pregnancy by inhibiting ovulation. The injection contains a synthetic version of the hormone progesterone, which is naturally produced in the body by the ovaries. In addition to preventing ovulation, contraceptive injections also trigger a thickening of cervical mucus that suppresses sperm’s ability to move through the uterus. If a sperm is unable to reach and fertilize an egg cell, then pregnancy cannot occur.
The birth control pill, more commonly known as “the Pill”, is a hormonal contraceptive tablet that is taken daily to prevent pregnancy. There are two types of birth control pills, combination pills, and progestin-only pills. Both forms of the pill contain hormones that regulate ovulation to prevent pregnancy.
|
Categories
All
Archives
June 2024
|
|
|
Donate to Male Contraceptive InitiativeYour generous donation makes a difference!
|
© Male Contraceptive Initiative. All rights reserved.























 RSS Feed
RSS Feed
