|
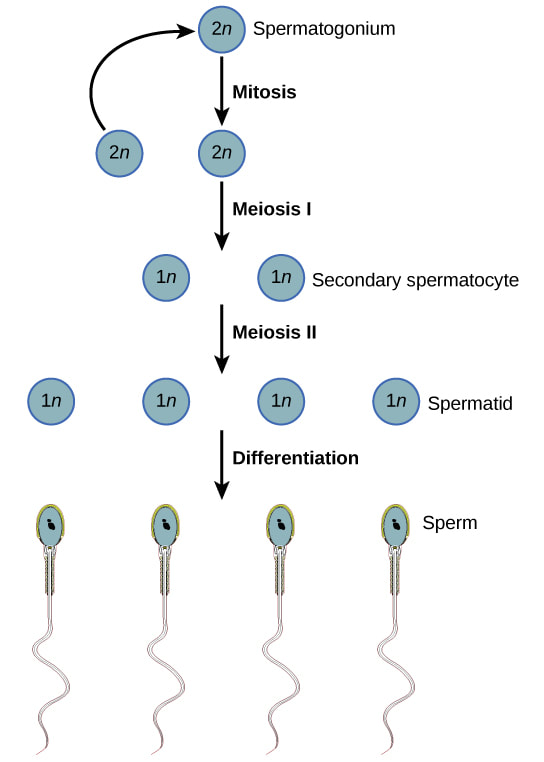
The human reproductive system is a complex set of intertwining factors, many of which are required for sustained fertility. By interrupting even a single one of these required processes, we can find new ways to create exciting non-hormonal contraceptives for men. One process is the creation of sperm, or spermatogenesis. No spermatogenesis, no spermatocytes, no spermatozoa, no sperm.Spermatogenesis is the creation of mature sperm from germ cells. Early-stage germ cells, called spermatagonia, reside in the periphery of seminiferous tubules of the testis. This population contains both stem cells and differentiating spermatogonia, which undergo a series of mitotic divisions to amplify the number of cells. Germ cells then enter meiosis, the second phase of spermatogenesis, and are called spermatocytes. During meiosis, genetic recombination occurs and spermatocytes undergo two divisions which halves the number of chromosomes present in each cell. The process of spermatogenesis, which starts with a spermatagonial stem cell, and ends with multiple fully formed sperm cells. Photo adapted from OpenStax College distributed under a CC-BY 3.0 license. During spermiogenesis, the final phase of spermatogenesis, haploid germ cells (spermatids) undergo extensive changes and become more like what we think of as traditional sperm, with tails and other structures like the acrosome. Finally, the non-motile spermatozoa are transported to the epididymis. Sperm undergo a maturation process as they transit the epididymis. As a result, they acquire the capacity for forward motility and become capable of fertilization. One way to influence spermatogenesis is through the manipulation of hormone levels. There are ongoing clinical trials focused on creating hormonal male contraceptives, but there are multiple non-hormonal approaches to stop spermatogenesis or interfere with epididymal maturation. A drug that stops spermatogenesis would have interesting characteristics, including a potential onset time of 2-3 months . This is because it takes quite some time for sperm to develop and get ready for action, and even after ceasing spermatogenesis, all of the existing sperm in the pipeline would still remain. MCI has funded projects in this space, such as Gunda Georg at University of Minnesota and her work on TSSK1/2. Other projects at institutions worldwide are focused on diverse approaches to temporarily disrupt spermatogenesis or epididymal maturation so that functional sperm are not produced. There’s more than one way to contracept.Reproduction is a big, complicated machine, with lots of ways to put a temporary hold on the process. Preventing spermatogenesis is one way that to make the next generation of male contraceptives. Other projects focused on preventing sperm transport, sperm motility, and fertilization are all being actively pursued. Together, we’re hopeful that these scientific ventures create multiple forms of male contraception with diverse product profiles that meet the needs of more users Nuts & Bolts: Spermatogenesis To learn more about, please visit our series of posts about male reproduction and contraception: For additional terminology related to male contraception and the male reproductive system, please visit our glossary: For additional publications related to male contraception and the male reproductive system, please visit our publications page:
0 Comments
Your comment will be posted after it is approved.
Leave a Reply. |
Categories
All
Archives
June 2024
|
|
|
Donate to Male Contraceptive InitiativeYour generous donation makes a difference!
|
© Male Contraceptive Initiative. All rights reserved.


 RSS Feed
RSS Feed
