|
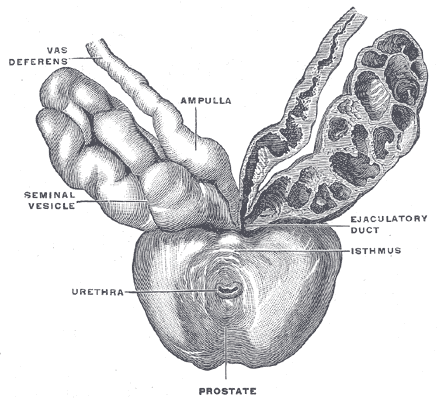
(Image courtesy of Henry Vandyke Carter, Public domain, via Wikimedia Commons) The seminal vesicles or seminal glands are two tube-like glands located between the bladder and the rectum, behind the prostate. Each vesicle consists of a 3-5 cm coiled tube containing multiple pouches.
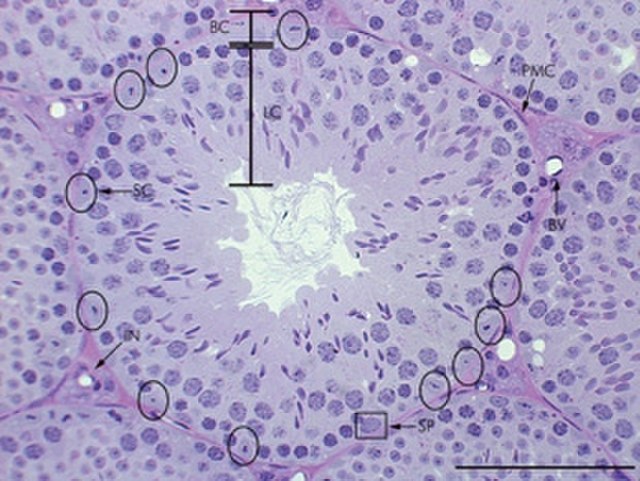
(Image courtesy of StemBook) The blood–testis barrier is a physical barrier between the blood vessels and the seminiferous tubules of the testes. The term is a bit misleading as it is not a blood-organ barrier, but rather one that is formed by the tight junctions between Sertoli cells of the seminiferous tubules. For this reason, this barrier is also referred to as the “Sertoli cell barrier”. The barrier isolates further developed germ cells from the blood.
Survey developed, conducted, and reported on by Edward Morris, Male Contraceptive Initiative Intern This survey was distributed through university students at a Southern US university (n=20, with 19 respondents completing the entire survey). Recruitment was done through a student group and other personal relationships and is not representative of any population.
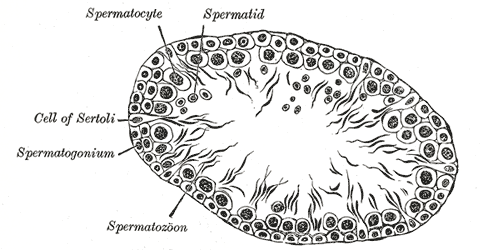
The aim of this survey was to understand the perceptions that this group of African American women have about potential future male contraceptive methods, and how their experiences with female contraception may potentially inform their perception of male methods. A secondary goal was to help inform future marketing efforts by understanding where participants get information on contraception and how they respond to that information. (Image courtesy of by Henry Vandyke Carter) Named after Enrico Sertoli, an Italian physiologist, Sertoli cells are a specialized cell type found in the testicles. Specifically, they are located in the seminiferous tubules of the testes and they facilitate the production of new sperm, or, spermatogenesis.
(Source: Public Domain) Also known as Cowper's glands (named for English anatomist William Cowper), the bulbourethral glands are two small glands in the reproductive system of male humans, and many male mammals, that produce and secrete a pre-ejaculate fluid called Cowper's fluid, known colloquially as “pre-cum”.
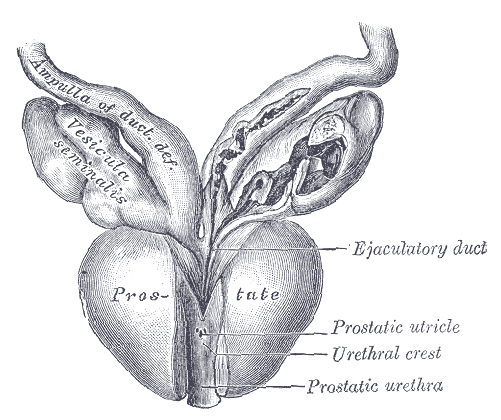
(Image source: Henry Vandyke Carter, in public domain) The ejaculatory ducts are a part of the male anatomy that allows the flow of sperm from the testes through the reproductive system and eventually out through the urethra.
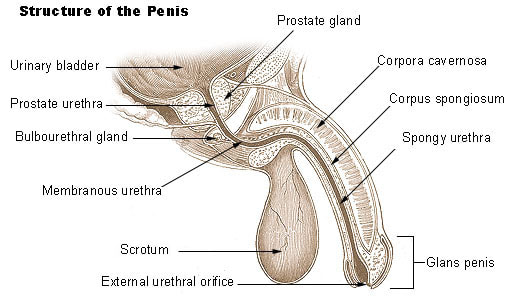
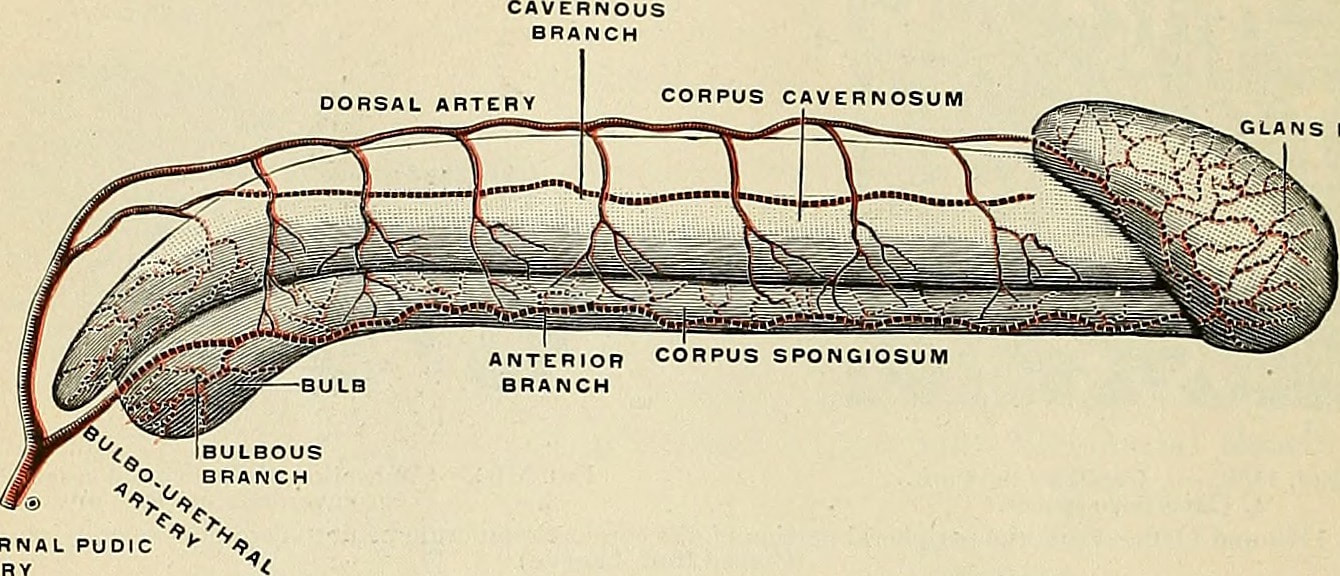
(Source: Internet Archive Book Images) The penis is the primary sexual organ that male animals use to inseminate females (or hermaphrodites) during copulation, or sexual intercourse. It is the male genital organ of higher vertebrates that carries the duct for the transfer of sperm during sexual intercourse. In humans and most other mammals, it consists largely of erectile tissue and serves also for the elimination of urine. It lies between the legs of a man, above the testicles.
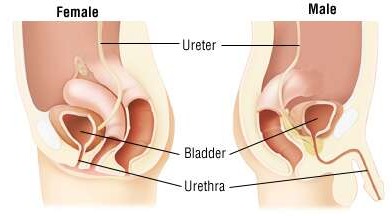
(Image source: Viva Differences) The urethra is a tube that connects the bladder to the urinary opening for the removal of urine from the body of both females and males. It is the vessel through which urine passes after leaving the bladder, and the conduit in men for semen during sexual intercourse.
Daniela (she/her/ella) is an MPH student at UNC Chapel Hill studying Health Equity, Social Justice, and Human Rights. She was drawn to MCI due to her passion for reproductive justice and sex positive education. During her practicum at MCI, she will be developing toolkit materials aimed at college students and young adults, as well as creating social media content and a social media engagement plan for the organization. What have you focused your studies on? How does that relate to male birth control?As an MPH student, I am focusing on health equity and am interested in equity within the sexual and reproductive health field. To me, health equity is inextricably tied to bodily autonomy; until everyone has the rights and access to healthcare, education, and resources to make informed decisions about their bodies, their lives, and their futures, then we will never truly have bodily autonomy. When it comes to deciding what does and does not happen to your body and your future, birth control has been incredibly important for millions of people over the last half century. However, we have a long way to go to ensure that everyone has a birth control method that works for them, which is what led me to work with MCI this summer.
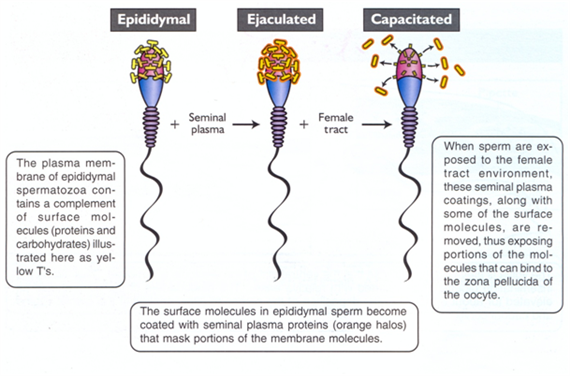
(Source: Ferenc Husvéth) Capacitation, generally speaking, is the change sperm undergo in the female reproductive tract that enables them to penetrate and fertilize an egg.
This step is a biochemical event; the sperm moves normally and looks mature prior to capacitation. It is important to note that once the sperm reaches the egg, it does not mean that it is capable of fertilizing it immediately. In order to fertilize the egg, the sperm must undergo the process of capacitation in the reproductive tract where a number of enzymes and signaling molecules are involved. This process can take around 10 hours, which means that the fertilization time is approximately 24 hours. (Image Source: Public Domain) We acknowledge that a person's sex and gender are two different things, as discussed here. Sex is defined as, "either of the two major forms of individuals that occur in many species and that are distinguished respectively as female or male, especially on the basis of their reproductive organs and structures."
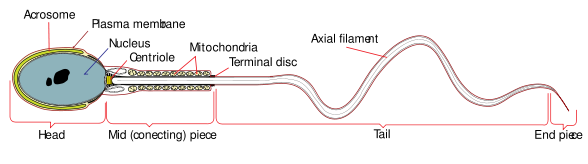
In this article, we will be referring to "male" and "female" in reference to the scientific classification of a reproductive system and not a person's gender identity. (Source: Wikimedia) In order to initiate fertilization, a sperm must first fuse with the plasma membrane of the female egg cell (known as the zona pellucida) and then penetrate through the membrane to fertilize it. Generally speaking, many sperm fuse to an egg cell, making it the “easy” part. Actually getting sperm to penetrate through the egg's external shell can, and often is, the more difficult activity. In order to accomplish this, sperm cells go through a process known as the acrosome reaction, which occurs in the sperm as it approaches the egg.
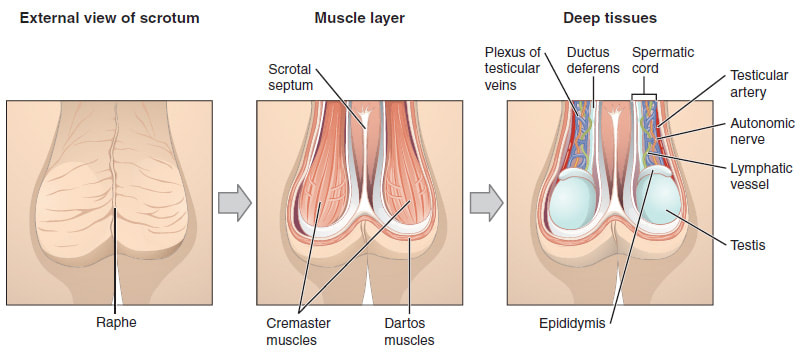
(Image source: Anatomy & Physiology, Connexions Web site. http://cnx.org/content/col11496/1.6/) The scrotum is a feature of the male reproductive system that hangs from the body at the front of the pelvis, between the legs. It is a sac of skin divided into two chambers, and it sits next to the upper thighs. The two compartments of the scrotum are distinguished externally by a middle ridge called the raphe. Internally, the raphe connects to a muscular partition, the septum, which serves to divide the scrotum into its two areas.
Our most recent intern from North Carolina Central University Edward Morris sat down with us to discuss his motivation in joining the team and his interest in male contraception. This blog post shares highlights from that conversation. Hello, my name is Edward Morris, I am a Public Health Education student at North Carolina Central University. I am a non-traditional student who had a prior career in the United States Army as a Bradley Commander and a Chemical Operations Specialist. I served 2 tours in Operation Iraqi Freedom. I wanted to continue to serve the American people and advocate for better health for underserved communities.
(Photo courtesy of Sansum Clinic) This blog post is written by Male Contraceptive Initiative's Youth Advisory Board Member Claudia Brewer When we hear “male birth control,” the vasectomy may be the first thing that springs to mind for many of us. Despite this, there’s a lot of confusion out there surrounding this procedure: Is it permanent, or reversible? Does it fulfill all of men’s contraceptive needs? To get to the bottom of these questions, I did some research and spoke with Dr. Alex Koper, a urologist at Sansum Clinic with 40 years of experience performing and counseling for vasectomies.
Male Contraceptive Initiative condemns in the strongest possible terms any and all acts of violence perpetrated against any group or individual. The most pressing reason for asserting this today is the unconscionable rise in attacks on people of Asian descent in America over the past year, with at least 3,700 individual acts of violence reportedly committed against this community since the start of the COVID-19 pandemic. We are saddened and distressed by this violence and the way it affects Asian American communities.
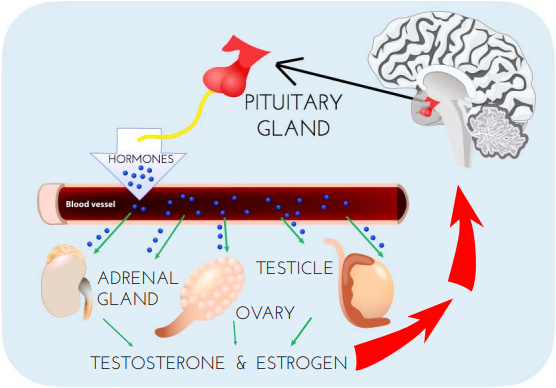
(Image credit: Dana Foundation - Illustration by Elizabeth A. Weaver II) Male Contraceptive Initiative provides funding and advocacy support for the development of non-hormonal, reversible forms of male contraception. But what does “non-hormonal” mean? How do these methods differ from “hormonal” contraceptives? In this post, we share a primer on the difference between hormonal and non-hormonal contraception.
A mandate for all physicians far and wide is “Do No Harm.” A mandate in which the health of the patient is prioritized above all else, and the health benefits of any treatment should outweigh the risks of that treatment. This creates a situation in which life-saving therapies with powerful and sometimes dangerous side effects are easily justified, because without treatment a very serious diagnosis could kill the patient entirely.
Our most recent MCI Youth Advisory Board member Claudia Brewer sat down with us to discuss her motivation in joining the board and her interest in male contraception. This blog post shares highlights from that conversation. What do you study/what's your academic background?I’m pursuing a B.S. in Molecular, Cell, and Developmental Biology with a Minor in Society and Genetics at UCLA. My goal in college is to gain a deep understanding of human health, from the complex molecular mechanisms underlying disease to the broader social and political implications of the latest bioengineering technologies. Most of my background is in biological research and healthcare. Most recently, I conducted research on a pathogenic protein associated with Alzheimer’s and other neurodegenerative diseases at the UCSB Neuroscience Research Institute. I currently serve as a scribe for a primary care physician at UCLA Health.
This blog post is written by Male Contraceptive Initiative's Executive Director Heather Vahdat, and is response to the article "The young women choosing to go without contraception" It’s Saturday and I’m supposed to be finishing a project that was meant to be a Christmas gift for my mother-in-law...last year. However, I allowed myself a quick look on the computer to find a sewing pattern I need and poof, here I am frustrated and writing a blog post. I can’t say I’m surprised that I find myself writing about contraception - it’s the classic “one quick peek at facebook/linkedin/wherever you saw the article couldn’t hurt”. But tell me, how can I not be distracted after seeing this article in my newsfeed?
Male Contraceptive Initiative’s mission is, “to empower men, and couples, to fully contribute to family planning goals by providing them the resources they need for reproductive autonomy.” It is how we articulate our most hopeful vision of the future: one where there is reproductive autonomy for all people. This vision and associated mission directs our daily activities, which encompass financial support to the male contraception research community and advocating for the development of additional male contraceptives.
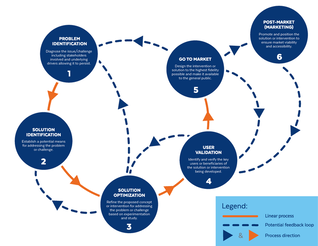
Introduction The drug development process is often presented as a linear process: you achieve one milestone before moving on to the next, with progress taking the developer ever forward. The Food and Drug Administration defines this process as such:
Based on the way that this information is conveyed, you might expect the process to visually represent something like this: Understanding people’s perspectives around male contraception helps guide our work at MCI. Sharing them is a privilege as well as a mandate: it’s of strategic importance to us to facilitate and broadcast the interest for male methods in an effort to present the undeniable market demand for them. Normally this is done through the lens of our grantees, fellows, research community, or even the general public. But lately, we’ve been endeavoring to share the views of MCI’s staff as well. In that spirit, this is a conversation with our Communications & Marketing Director Kevin Shane in which he shares his thoughts about male contraception as well as his interest in working with MCI.
Oleksandr “Sasha” Kirsanov is a PhD candidate in the Geyer laboratory at East Carolina University’s Brody School of Medicine. His work is focused on defining the mechanisms underlying spermatogonial differentiation and meiotic initiation. In this blog post, Sasha shares about his work in the field of contraception, what he hopes to learn as an MCI fellow, and the future outlook of male contraception.
Continuing our series sharing the thoughts and perspectives MCI staff has on male contraception, we sat down with our Program Coordinator Jaylan Weaver to hear his thoughts. Jaylan initially joined MCI as an undergraduate fellow, so he brings a unique perspective to a topic that means so much to all of us. In this post, he shares his motivations for working at Male Contraceptive Initiative as well as his thoughts about male contraception.
|
Categories
All
Archives
April 2024
|
|
|
Donate to Male Contraceptive InitiativeYour generous donation makes a difference!
|
© Male Contraceptive Initiative. All rights reserved.













 RSS Feed
RSS Feed
